October is Breast Cancer Awareness Month. The campaign aims to raise awareness of the disease, educate about its symptoms and prevention, and fund research into causes, treatment, and cure. This year’s focus is on metastatic breast cancer, where the cancer has spread beyond the initial tumour site of the breast and into other parts of the body.
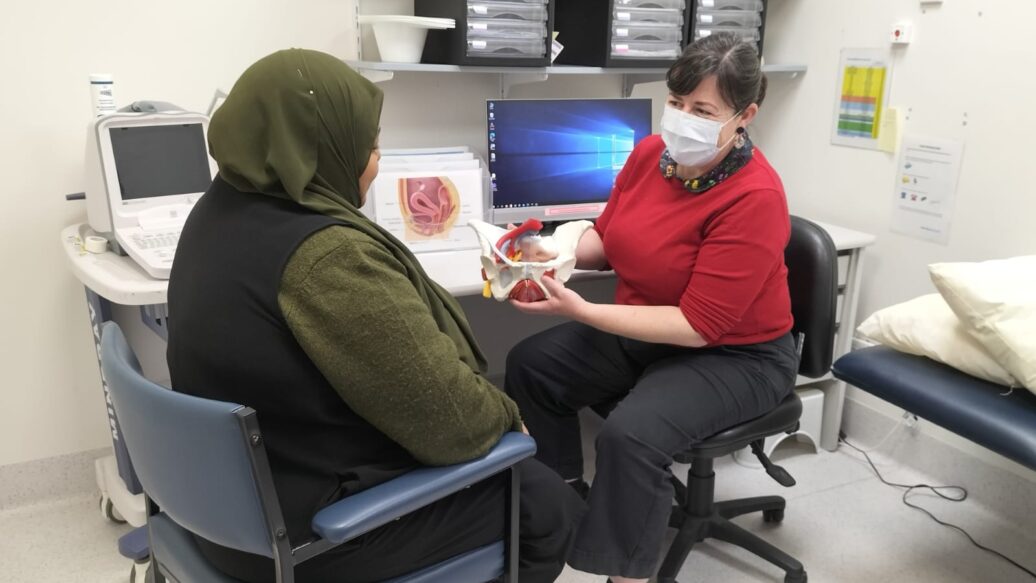
Melanie Bullock, McGrath Metastatic Breast Care Nurse Consultant (MBCN), who is based at Northern Hospital Epping, said, “Diagnosis rates continue to rise, but so has the survival rate. It’s all about early detection.”
Australia has one of the best breast cancer survival rates in the world, with 87.4 percent of people diagnosed surviving at least 10 years.
“Our team has grown to match the needs in the community,” Cheryl Murray, Breast Cancer Nurse Consultant added.
“As patients live longer, the duration of the specialised care they require to navigate their path to recovery naturally increases too. Northern Health now has three breast care nurses, allowing for a wider support service, including metastatic patients.”
Understanding the need for a multi-disciplinary approach for effective care, the team has organised an ‘Introduction to Breast Cancer’ study day for all Northern Health staff to be held on Thursday 17 October, 8 am – 2 pm in person at NCHER Lecture Theatre 2. Staff can Register Here.
The study will include topics on:
- Patient journey from diagnosis to treatment
- Treatment options
- Supportive care of the patient, and much more.
To facilitate early detection, BreastScreen Victoria provides free mammograms to women and trans and gender-diverse people with no breast symptoms.
- Women and trans and gender-diverse people aged 50 to 74 should be screened every two years.
- Women and trans and gender-diverse people aged 40 to 49 and over 75 are also eligible to receive a mammogram with BreastScreen Victoria every two years, however, it is encouraged to speak to a doctor to see if breast screening is the right option for you.
To schedule your free breast screening appointment, please visit Breast Screen Victoria or call 13 20 50 for more information.
Pictured in featured image: Breast Care Nurse Consultants, (L-R) Sarah Young, Cheryl Murray and Melanie Bullock.