This week, we are celebrating Occupational Therapy (OT) Week, and given the onset of droughts, bushfires, and the global pandemic, in 2020, the theme of this year’s OT Week is Resilience: Supporting our communities to rebuild, recover, and reengage. In supporting people to participate in activities they find meaningful, occupational therapists are vital in helping our communities through disaster recovery.
Occupational therapy provides practical support to empower people to facilitate recovery and overcome barriers preventing them from doing the activities (or occupations) that matter to them. An occupational therapist will consider all of the patient’s needs – physical, psychological, social and environmental – with the ultimate goal of supporting individuals to increase their independence and satisfaction in all aspects of life.
Renee Catton, Senior Occupational Therapist, highlighted the importance of OT professionals during the pandemic by sharing a recent patient story, where the team worked with an elderly patient in the GEM Ward at Bundoora Centre, who wanted to spend some time at her daughter’s home before going back to her facility.
“Both patient and the family felt that her mood would improve if she spent some time at home with her daughter, and this was her huge wish. The OT department was given 48 hours notice to facilitate the interventions required to support the patient and daughter’s wishes,” she explained.
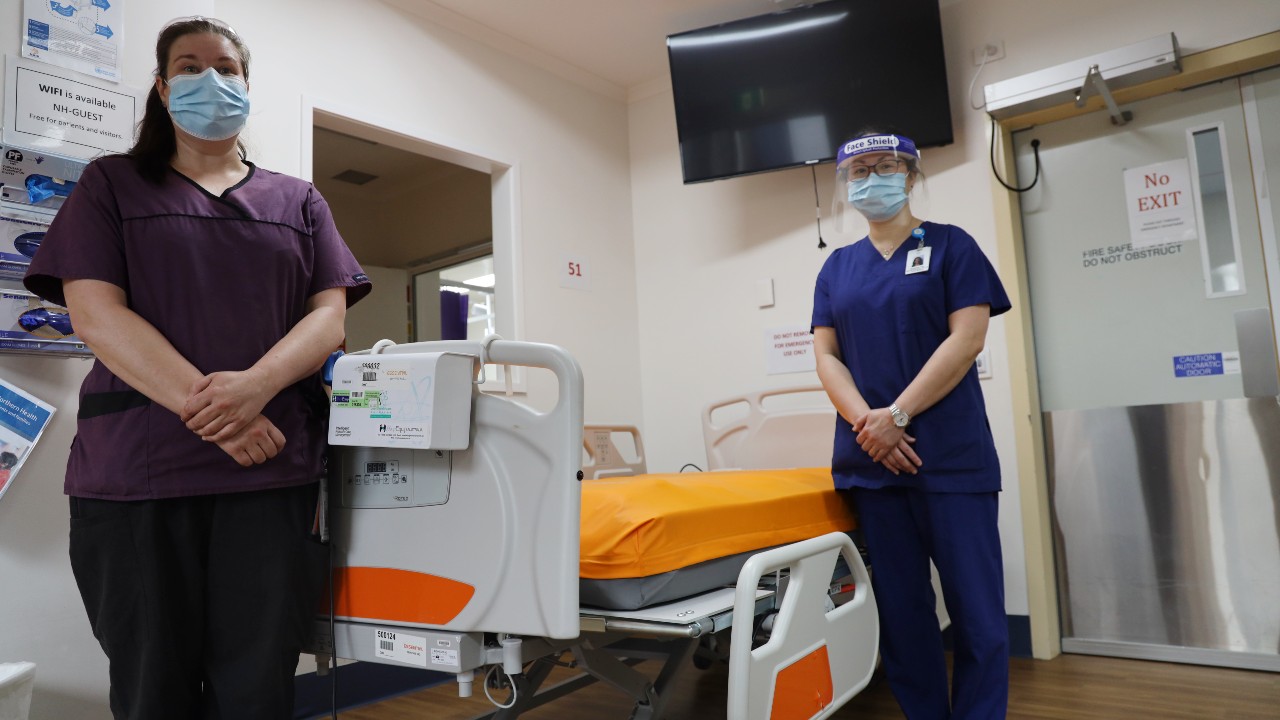
For this patient, our OT team provided carer training for management of all functional mobility and management of personal care, including how to safely use a hoist, education on strategies to best prevent pressure injuries and falls, and arranging the hire of extensive equipment to support the patient’s high care needs such as a hospital bed, pressure relieving mattress, hoist and sling, wheelchair, pressure relieving cushion and commode.
“All of this was completed and the patient was discharged home in under 48 hours of plan and goal being developed,” Renee added.
The family was grateful for the help and were thankful she was able to spend some time with them. Here are the words from the patient’s daughter:
“Thank you so much again for all your assistance in helping us to get mum home for a break before she returns to her aged care home. Time has flown by and we have all had a great time together.”
“The great work that the team did really reflects this year’s motto in supporting our patients to rebuild, reengage and recover,” said Renee.
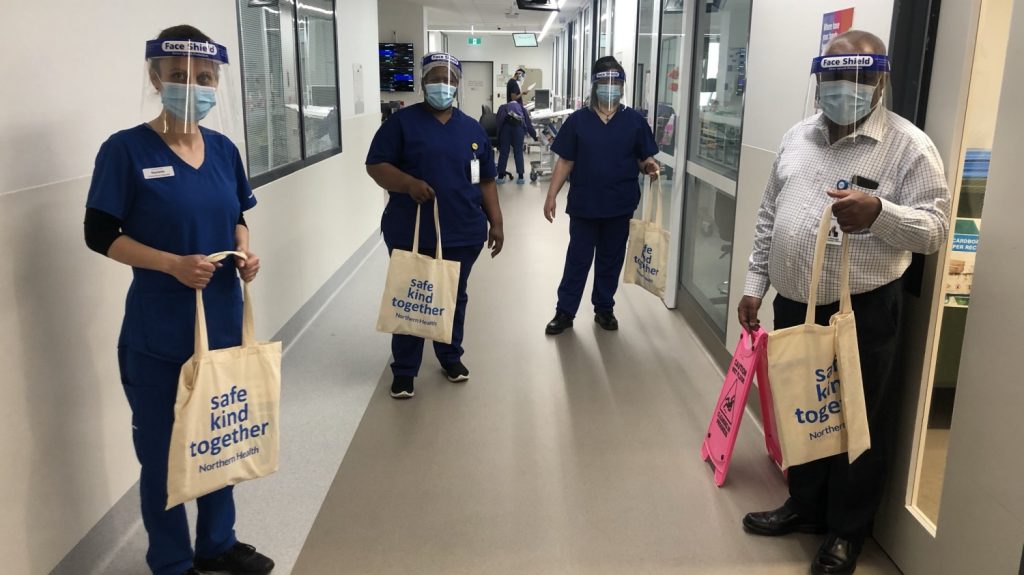
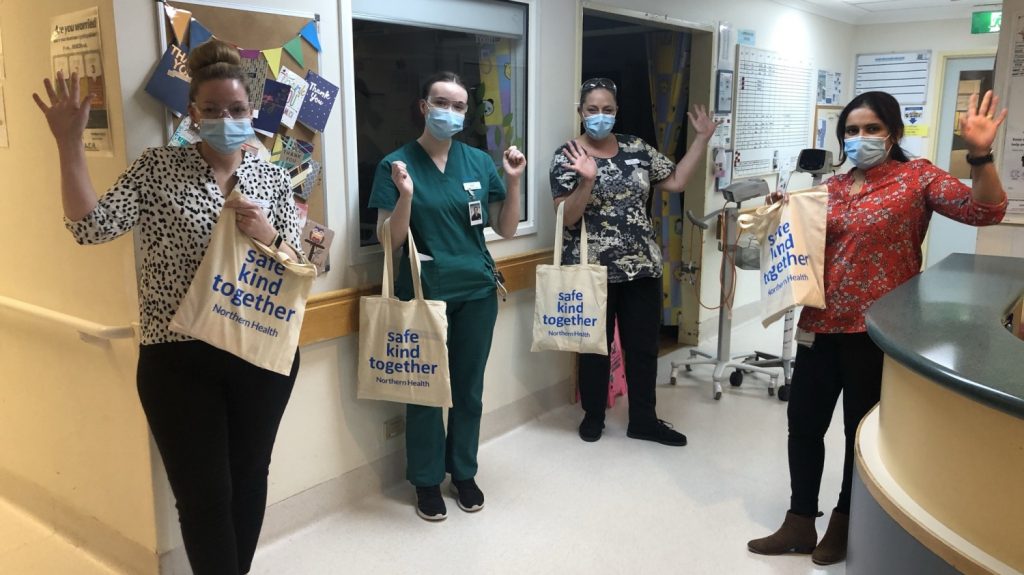
Featured Image: Bundoora Centre OT team