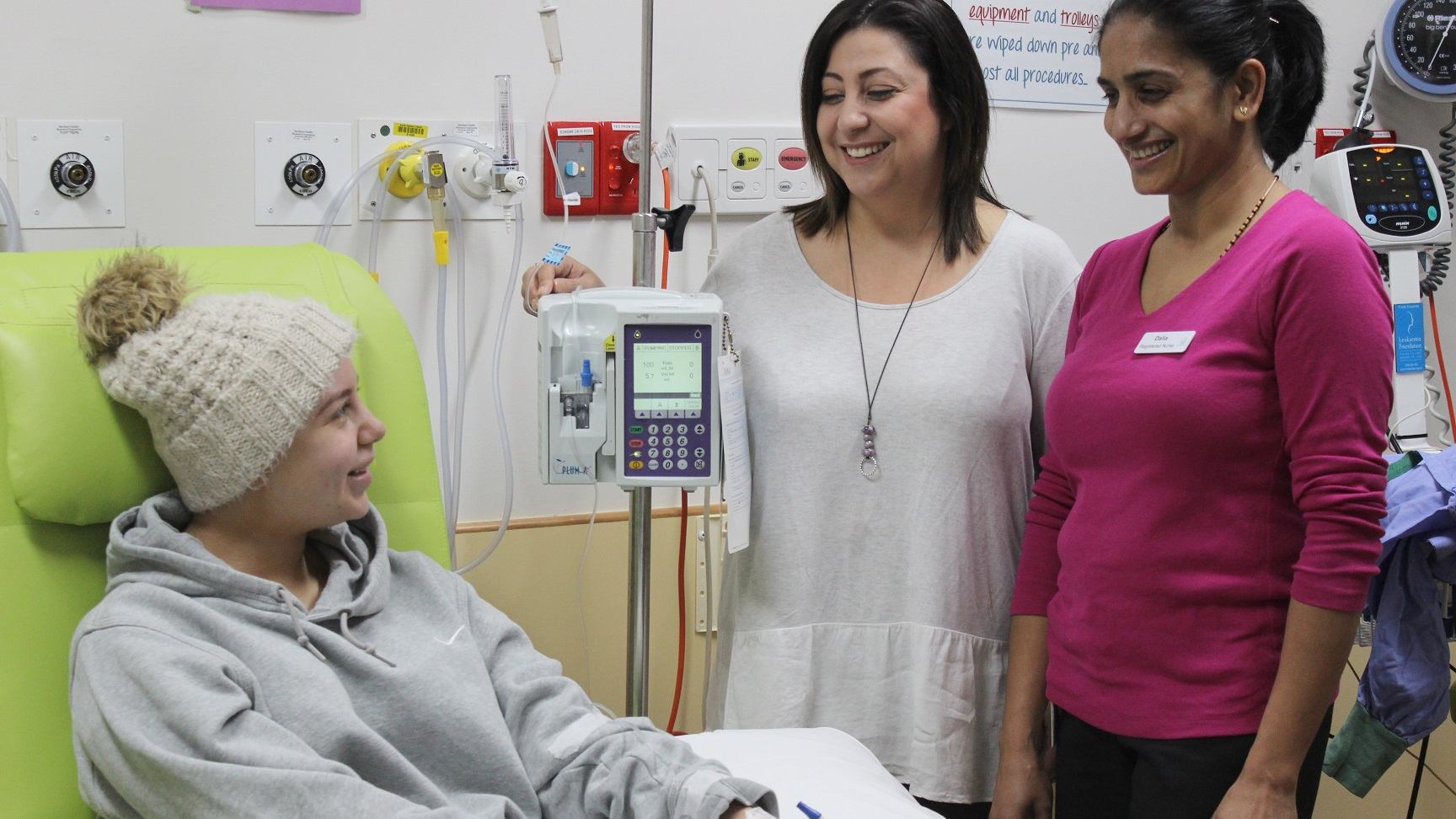Our Day Oncology Unit recently received a grant from the Northern Health Foundation for a treatment chair and two privacy screens, which will greatly improve patient experience and help to replace aging equipment.
Day Oncology Nurse Unit Manager, Melissa Gwynne, says the unit have been working towards replacing their older chairs for a number of years, and have been able to achieve this with the support from the Northern Health Foundation.
“The chairs we currently have are over ten years old, quite big and cumbersome, and not as comfortable for our patients,” Mel explains.
“The new chairs are slim line and are lighter – they’re actually easier for the nurses to maneuver around and put patients into resus position if needed.”
Mel tells us that patients will benefit greatly from the new treatment chairs – “they’re much more comfortable to sit in – the patient feedback has been really great – and they’re a brighter colour as well.”
The additional privacy is another feature patients will benefit from.
“The Day Oncology Unit is very open, and we don’t have curtains between chairs. When a patient requires some privacy, it will be really nice to have screens to provide that much needed privacy,” Mel says.
“The screens we are getting are quite compact and infection control compliant,” she adds.
Mel says family members will also benefit from the lighter, more compact treatment chairs.
“Because they’re smaller than the older chairs, it means more family can fit in the room and sit with their loved one,” she says.
When asked what it meant to the unit, Mel says, “It really means a lot – we’ve been very lucky when it comes to donations from our sponsors and without the Northern Health Foundation, we would be unable to do it,” she adds.
“They do a lot for us, and when the donors come in and see what we’ve done, they’re really happy. We get a lot of feedback and ideas from patients about what they want, so that really helps.”
Longtime Northern Health supporter and board member of the Northern Health Foundation Board, Trudi Hay, made this donation possible after raising $9,000 from her annual High Tea event.
The Northern Health Foundation is a philanthropic and fundraising arm of Northern Health and aims to raise $4 million for equipment and research between now and 2021.