On behalf of the Board and Executive Team, thank you very much for your commitment and professionalism during 2020. This year has been completely different to anything we’ve seen before.
Staff had to change the way they work, whilst making sure patient care continued at the high standard expected of us. Many staff put their lives in danger to continue to provide this care.
We did not get everything right – but we adjusted quickly. We were learning all the way though the pandemic, and then the experience of the second wave taught us more.
In early July, when there was infection within the emergency department, one group was furloughed – while the other group still stood up, irrespective of the risk, and worked through until the first group came back.
Similarly, when our specialist units were furloughed, others picked up the load of the unit and kept the patient care going.
At the peak of COVID-19, Unit 1 staff from Broadmeadows Hospital came across and supported the Northern Hospital SCOVID (Suspected COVID) Ward 15. Staff were prepared to leave their normal ward to work in a high risk area where the need was greatest.
Our Infectious Diseases Unit expanded and provided comprehensive care for our patients, as well as supporting our frontline clinical staff on how to manage the risk during this difficult period.
One of the early challenges was sourcing large quantities of the PPE we needed. Our Procurement and Supply team worked around the clock to source daily deliveries of the broad range of protective equipment available to clinicians.
In addition, early in the pandemic, we had very limited COVID-19 testing capacity. Our Northern Pathology Victoria service quickly adjusted with initiative after initiative to expand their testing capability to over 1,000 per day – with some of the fastest testing times in the state.
We were the first health service with wide-spread infection, with our emergency department and ward staff caring for many older patients with COVID-19. Our early experience and learnings have been adopted by other health services – and they have shared their experiences with us.
Our Residential-In-Reach team worked in multiple challenging private aged care settings, helping many residents avoid being transferred to hospital – taking them away from their familiar environments.
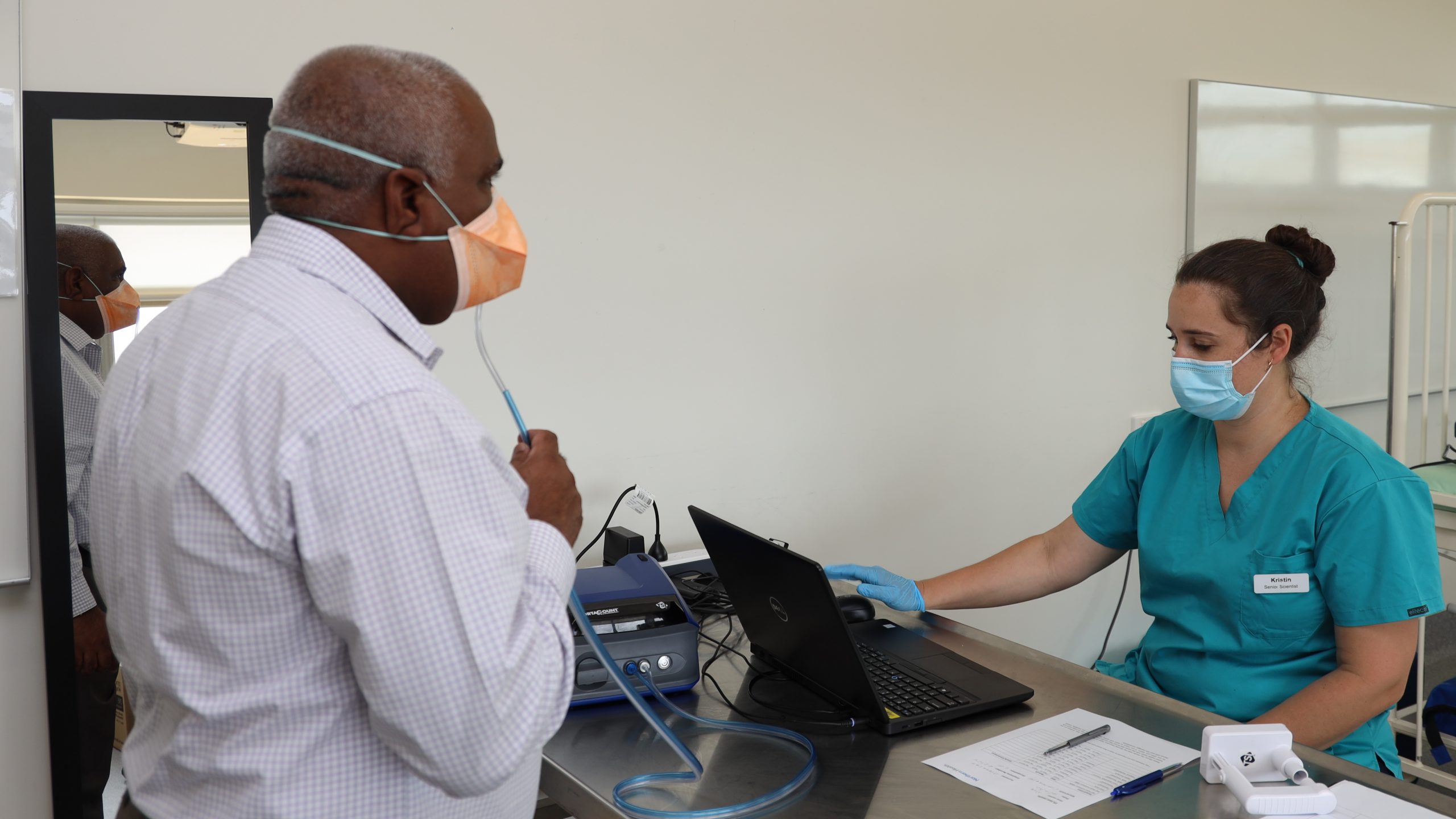
Northern Health was chosen to conduct the first fit testing pilot with 800 frontline staff. Now the pilot is complete, we are testing different types of masks so that the Government can broaden the supply of N95 masks from several sources, rather than relying on a narrow selection.
We had to reduce face-to-face specialist clinics and rapidly accelerated implementation of telehealth – a positive option for the majority of our outpatients into the future.
One of the cornerstones of our strategic priority of a Healthier Community – is Staying Well. This is where much of our service expansion will be either home-based care or virtual, rather than people coming into hospital. During the peak of the COVID-19 period, we had to adjust the way the team were working to look after COVID-19 positive people in the community. Now, Staying Well resumes – aiming to enrol 1,000 of our chronically ill patients to the program in coming months.
Another challenge in health is to catch up on deferred care – where we had to place much of our elective surgery and outpatients on hold to create capacity to deal with COVID-19. Additional work with these patients will commence in February, whilst we maintain our vigilance for any flare-up of COVID-19 in Victoria – before vaccines are readily available.
Looking ahead to 2021, we have multiple infrastructure projects commencing or nearing completion. Stage 2 of the South East Block is progressing on target, with the new wards and theatres to be commissioned by around March.
The Victorian Government has announced additional mental health beds in our region, in response to the Mental Health Royal Commission’s Interim Report. Planning has commenced for 30 additional beds that will be built on the front car park at Epping, adjacent to the emergency department. Construction will commence in 2021 with completion in 2024.
Planning for new community hospitals at Craigieburn and in the City of Whittlesea has commenced. Construction of the Craigieburn Community Hospital will commence in 2021 on our Craigieburn Centre site. The Victorian Government has set aside funds in the recent budget to purchase land in the City of Whittlesea.
Our Renal Dialysis service has been functioning out of a portable for a very long time. We are converting the old Clinic E into a Renal Dialysis Unit by May. This will be a much better environment for the patients’ experience – and closer to critical care back-up if required.
Early in 2021, we will commence building our new 1,000 car multi-deck car park at Epping, to accommodate additional convenient on-site parking for staff.
We are currently building a new IT server room to be completed by May, with new modern equipment replacing outdated equipment currently located in portables. We are using this move as an opportunity to move 50% of our existing IT network to a cloud based environment. This new infrastructure will help support our EMR implementation, which will be another key focus of the organisation over the next three years.
I encourage as many staff as possible to take time off between now and Australia Day, before we get capacity back to normal in February.
Thank you all again for your work during 2020. I hope you enjoy the festive season taking a well-deserved break – and please stay safe.
Siva Sivarajah
Chief Executive