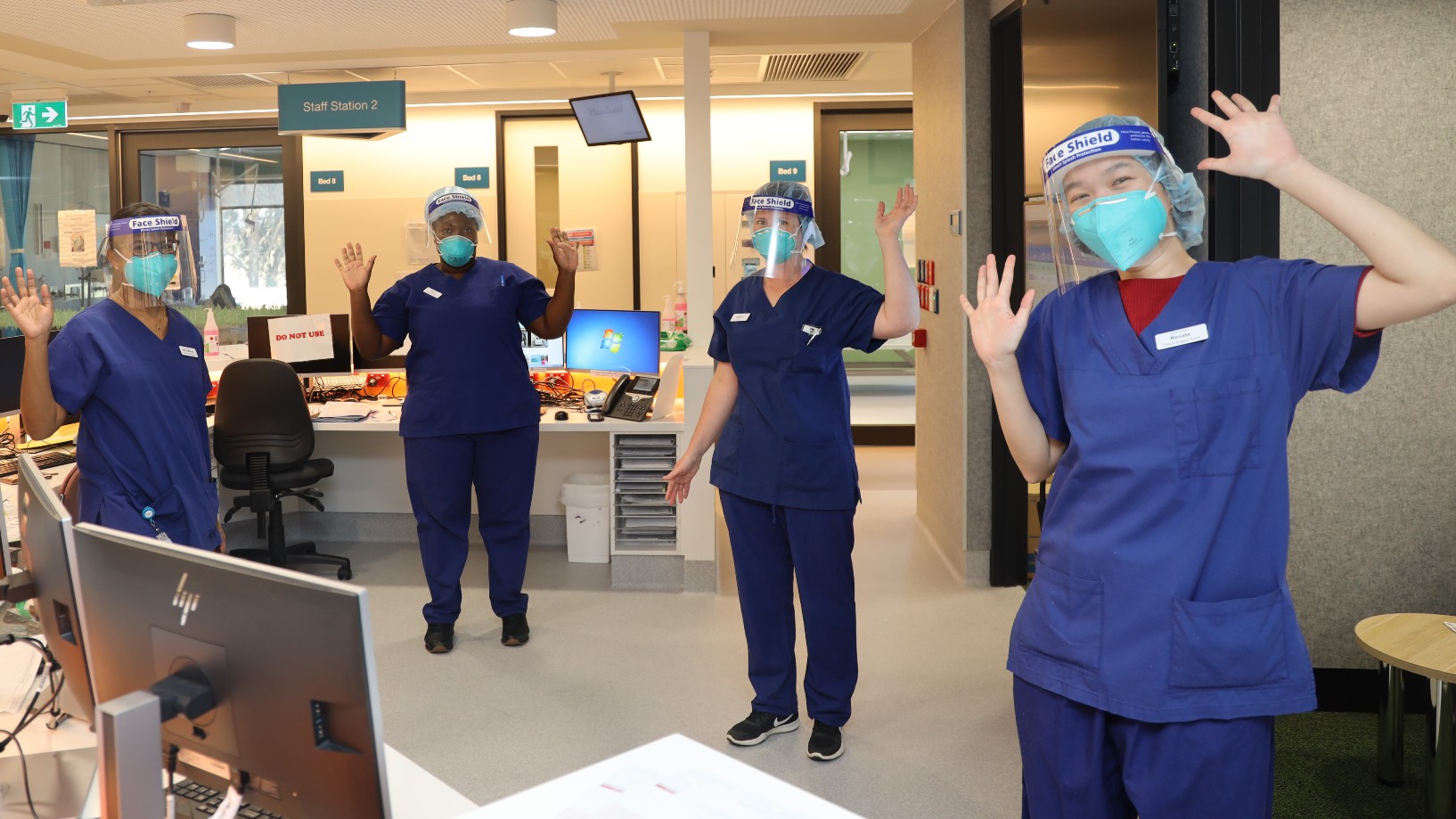
In the last week of July, Unit 1 staff from Broadmeadows Hospital were redeployed to the new Ward 15 at Northern Hospital Epping – to look after COVID-19 positive and suspected COVID-19 patients.
Minu Manuel started her Nurse Unit Manager role at Unit 1 just the week before. She didn’t get much time to enjoy her new role, as the COVID-19 numbers were rising.
“It was a very short notice for our staff and a big change, but the staff turned up for work the next day and embraced it. Some of them hadn’t been at the Epping campus for years, so working in this new environment was very brave of them. The months from July onwards were very challenging times for any health care worker,” she said.
Unit 1 at Broadmeadows Hospital is a surgical and medical ward, and the staff are used to overnight stays of surgical patients. The move to Ward 15 for them meant adapting to wearing PPE at all times, making sure they adhere to all COVID-19 precautions, upskilling in different patient conditions and procedures quickly, and adapting the care according to infection prevention principles.
“The first thing staff had to learn is how to be in the N95 mask all day, and in full PPE. Another big challenge was getting to know how the Epping campus works, as surgical and medical teams are different here, and just getting accustomed to a new environment,” she said.
Minu says her team received huge support from the access team, being a fast-moving ward, and also working closely with NUMs of surgical division and Linda Romano, Divisional Director.
“I have been extremely pleased and thankful for all the hard work and resilience from the Ward 15 staff. It was certainly a big change for most. However, despite their initial reservations, they were all committed to providing high quality and compassionate care to our community during such challenging times. Their contribution assisted greatly in Northern Health’s COVID-19 pandemic response, and for this, I will be forever grateful,” Linda said.
The team and Minu also highlighted the support from multiple departments – “We had Grant Taylor, Director of Nursing and Operations for Broadmeadows Hospital supporting us the whole way through this redeployment and guiding me as the new NUM. We also had huge support from nursing education and infection prevention, who were with us on the ward. In the moments of high stress, staff were given the opportunity for TREAT sessions and EAP, and many staff have taken advantage of it. Now that it has been four months working on Ward 15, the team has adapted to the change and knows the system,” she said.
Grant Taylor said he is exceptionally proud of the Unit 1 team.
“The team have demonstrated the Northern Health value of together, both in supporting each other, as well as their colleagues at Epping during what was a very challenging time for Northern Health and the state of Victoria as a whole,” he said.
Richard Ram, NUM for Ward 15 and 16 added: “The team from Ward 15, during the second wave of COVID-19, has shown the values of Northern Health, and this has resonated daily in their operations. Great team comradery from the Broadmeadows team whilst at Epping”.