In 2022, Northern Health, in partnership with Swinburne University and Medibank, were successful in obtaining a Workforce Training and Innovation Fund (WTIF) grant from the Department of Jobs, Skills, Industry and Regions for close to $2.4 million to create a new Certificate III in Community Services (Health Navigation).
In a 2022 policy brief on patient navigators, the World Health Organisation (WHO) highlighted key programs globally where peer health navigators have not only overcome barriers to care for vulnerable and disadvantaged groups, but have increased prevention and health promotion within hard-to-reach communities. However, the policy brief also highlighted that existing programs varied in terms of context and setting, overall aims, practical implementation, the role itself, and the skills and training required.
The WTIF grant has provided Northern Health an opportunity to position itself as a leader in a field that is fast becoming recommended practice. The 2023-2033 Australian Cancer Plan identified health navigation as a priority area for action. At the same time, Northern Health was developing a similar initiative with colleagues from Peter Mac. In December 2023, the final report of the Independent Review of the National Disability Insurance Scheme (NDIS) also identified the need for all people with disability to have access to a health navigator.
Dr Rebecca Jessup, Director of Research and Evaluation of the Staying Well Program and Principal Investigator on these projects, says, “Integration and cooperation within the health system and employment within health care services have been identified as one of the most important enablers for these roles. Positioning this work within a health care organisation is critical to ensuring adoption of the roles into practice.”
Peer health navigator roles may include providing patients and communities with information about their conditions to support self-management, providing more holistic patient-centred care, identification and resolution of barriers to health care, and linking individuals and communities into health and social services. Peer health navigators may work in disease-specific e.g. cancer, HIV, cardiovascular disease, mental health, setting-specific e.g. emergency departments, primary health care, or more general navigation roles.
Internationally, health navigator roles have been found to reduce emergency department presentations by 23–51 per cent and hospitalisations by 21–50 per cent. Studies in migrant communities have found that peer health navigators improve adherence to chronic disease care, increase cancer screening up to 24 per cent, and result in significant improvements in exercise and dietary habits. Shared experience, culture and language are key contributors to the impact of peer health navigators on health care engagement and improved patient outcomes for migrant communities.
“In line with the 2022 WHO policy brief, there is a need for an agreed level of capability and competency in the Australian context to develop appropriate training curriculums and vocational programs for these roles, in conjunction with delegation and supervision frameworks” says Dr. Jessup.
“In association with Swinburne University and Medibank, I am excited that we are addressing this gap in Australia and doing work that will genuinely benefit our community.”
The WTIF is a targeted, Skills First funding stream. WTIF creates opportunities for the joint exploration of new ideas and solutions to enhance workplace productivity and employment growth in priority industries identified by the Victorian Government, in collaboration with industry partners and Skills First training providers.
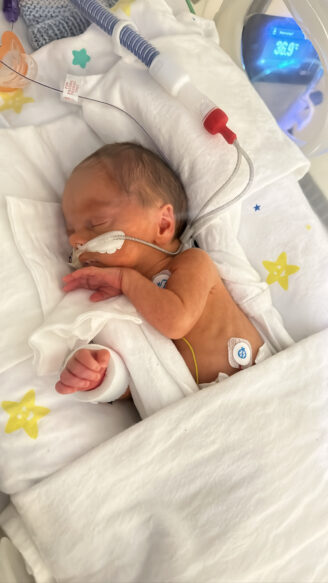
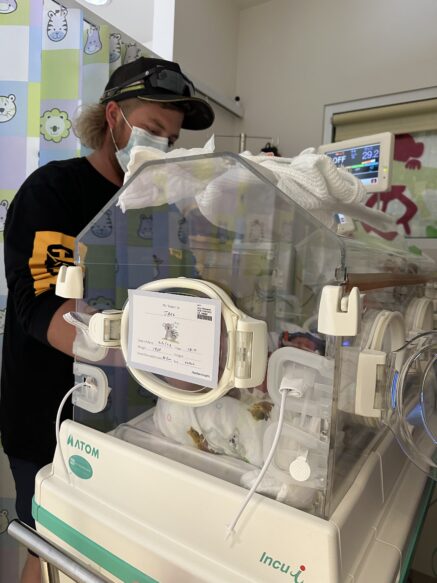
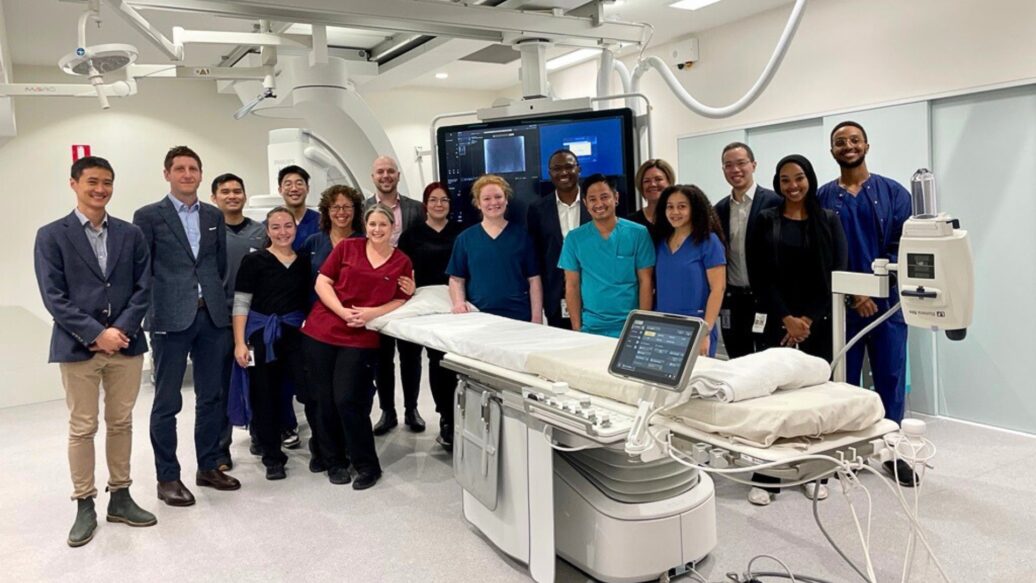
Pictured clockwise from top left: Northern Health peer health navigators for Pasifika and Arabic speaking communities; at the Victorian Arabic Social Services, Broadmeadows; celebrating Pacific Island Women’s Health Equity Day.