IDAHOBIT stands for International Day Against Homophobia, Biphobia, Interphobia and Transphobia.
The day is celebrated across Australia and is a day where we take a stand against discrimination and support lesbian, gay, bisexual, transgender, intersex, and queer (LGBTIQ) friends, colleagues and families. HOBIT can occur online, face to face and can make people feel unsafe, and like they cannot be themselves. Sexuality, gender identity or intersex status are not always visible and we are responsible for creating and maintaining a culture where everyone feels safe and included.
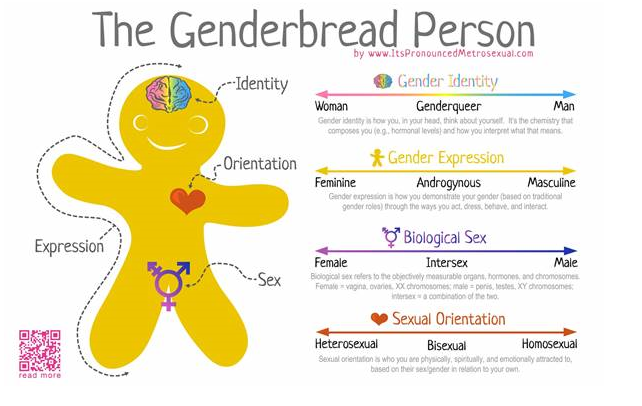
This Friday, Northern Health is holding the Inaugural ‘Genderbread Person Bake-Off’, which will take place in the Northern Hospital Foyer at 12 pm. This will be followed by two Information Sessions at 1 pm and again at 2 pm at NCHER (Click to book). We are pleased to announce that these sessions will be delivered by a prominent GP / LGBTI Health Expert, Dr Ruth McNair.
Dr McNair specialises in lesbian and bisexual women’s health, transgender health, mental health and wellbeing, and is an Honorary Associate Professor at the University of Melbourne, teaching LGBTI community research.
Jason Cirone, Director, People & Culture is encouraging all to grab their multi-coloured food dye and enter the Genderbread Bake-Off.
“The judges will be looking for the most creative concept of the Genderbread Person, which will be delicious, colourful and represents inclusivity of LGBTIQ people, and awarding prizes on the day,” Jason said.
So get baking and drop off your ‘Genderbread Person’ at the People & Culture Office, which is located on the ground floor (next to the library) between 8.30 am and 10.30 am. Judging will take place at 12 pm in the Northern Hospital Foyer.
Staff are encouraged to wear a rainbow ribbon, pin or piece of clothing on the day.