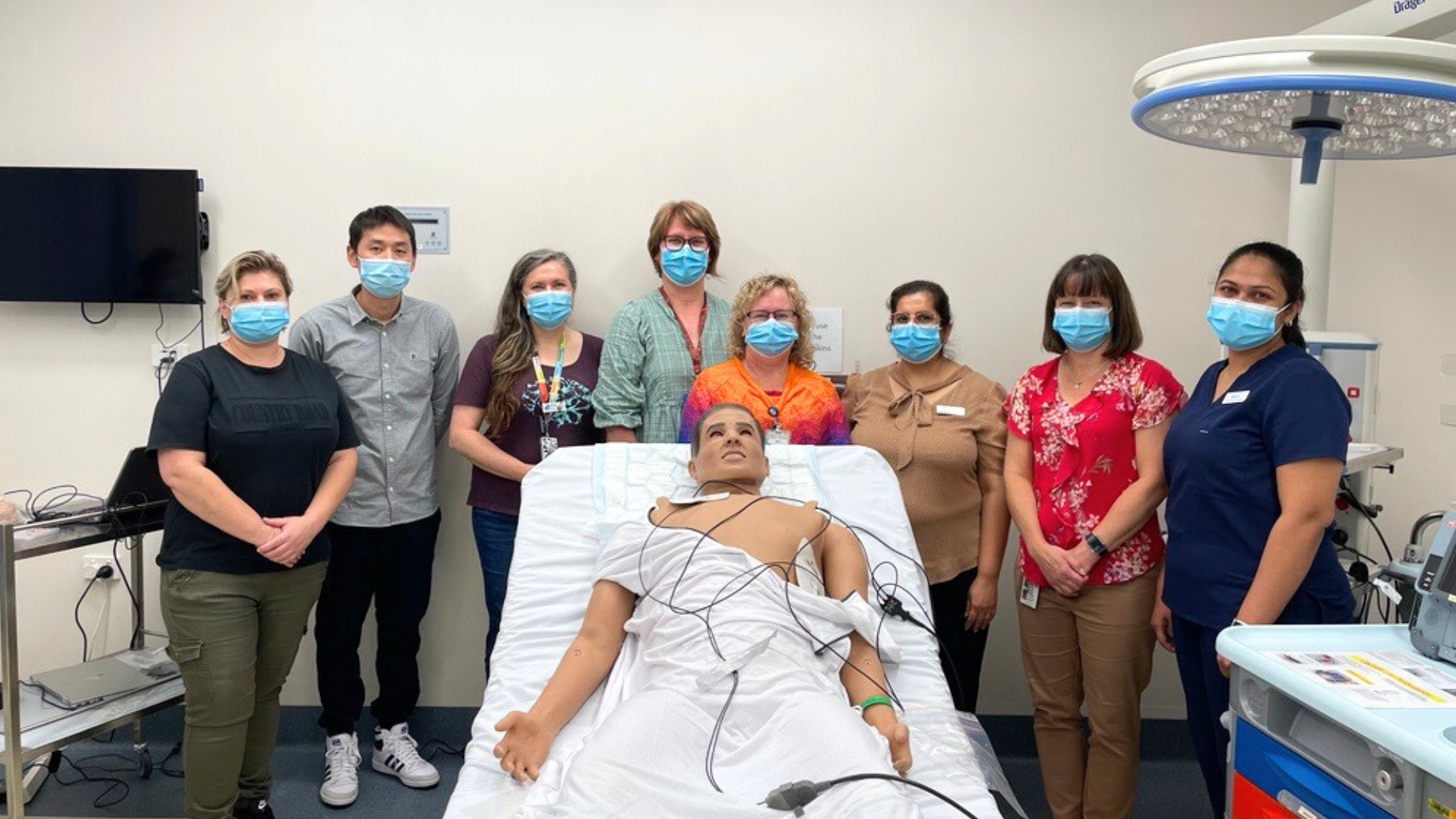
Northern Health has recently welcomed a new team member in Simulation Centre – a new generation SimMan 3G manikin.
The manikin was purchased conjunctively by Northern Health, the University of Melbourne and Latrobe University, and will provide base education, simulation and training for Northern Health staff and students.
The Simulation Centre is also equipped with two older models of electronic SimMen, IV equipment and cameras to provide students and staff with education and training opportunities.
The new SimMan 3G manikin is a more advanced model than its predecessors, featuring functions such as a highly realistic look and texture, the ability to speak and project a trainer’s voice via a headset and a microphone, various pre-programmed voice-controlled commands, and even the functionality to cry.
“The SimMan 3G plus has the most realistic patient presentation features. I am looking forward to including SimMan 3G plus in clinical deterioration simulations across the hospital. This will give the learners a real experience and enable them to practice working within the multidisciplinary team in coordinating care during clinical emergencies,” said Clinical Nurse Educator Simulation and Clinical Support Nurse Surgical, Navya Jose.
Consultant Anaesthetist, Andrew Huang, says having an advanced model available at Northern Health will significantly improve the training opportunities for staff and students.
“The additional training capacity with the new model has really opened up the possibility to create high fidelity education opportunities for our students and staff to enhance the care we provide at Northern Health,” he said.
The SimMan 3G manikin can be used by medical, nursing or allied health educators for, but not limited to, deteriorating patient scenarios and cardiac arrest resuscitation scenarios.
“Students have already said how much more realistic he is. I have used him for deteriorating patient scenarios, and they were much easier to run. The system gave me excellent feedback of CPR effectiveness. The students found being able to have measurable outcomes in CPR, and improvement, very rewarding,” said Dr Pip Wills, Simulation Teaching Specialist, University of Melbourne and Emergency Physician, Northern Health.
Monika Aulakh, Lecturer at La Trobe University says that SimMan 3G will help students to minimize making mistakes in their future practice.
“SimMan 3G plus can provide students with a learning environment to develop nursing skills, that is safe and controlled so that the participants are able to make mistakes, correct those mistakes in real time and learn from them, without fear of compromising patient safety.”
The new SimMan 3G manikin is available for simulation and training sessions Monday – Friday, across all four campuses of Northern Health. To book a session please email simulation@nh.org.au
Pictured (L-R): Sarah Rexhepi, Simulation Technical Support Officer, Dr Andrew Huang, Dr Suzy Cook, Lorette Botha, Dr Pip Wills, Monika Aulakh, Eloise Willams and Navya Jose with the new SimMan 3G manikin.