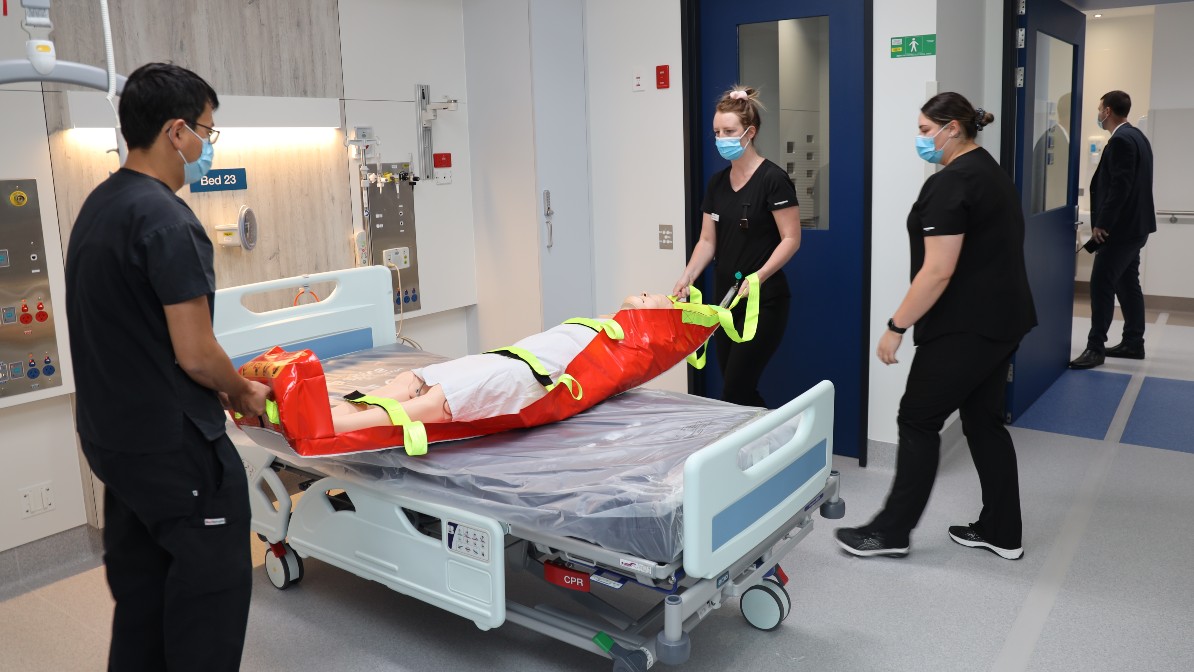
Long-stay patient, 57-year-old Mark Lazaric (pictured above with ICU staff), recently visited the Northern Hospital Intensive Care Unit (ICU) to say thank you to the staff that cared for him during his 43 days in ICU.
Mark spent a total of almost three months admitted to hospital during one of the most challenging times our health care staff have ever faced – during the height of the COVID-19 pandemic.
After suffering a major heart attack while walking his dog in August last year, Mark was rushed to Northern Hospital Epping. This week, Mark celebrated an amazing accomplishment – he was back at work for the first time since the heart attack.
Mark doesn’t remember much from the first five days in hospital but said, “the doctors had their work cut out for them.”
“I do remember opening my eyes and having six doctors looking at me, and I was confused where I was,” he explained.
During his ICU stay, Mark felt assured in his recovery from the dedicated team caring for him.
“I had a nurse sitting at a station watching me 24/7 for 43 days – they didn’t leave me by myself the entire time I was there. It showed their massive commitment,” he said.
“I’d never really been to hospital before so I didn’t know what to expect but I was blown away, they’d come in and have a chat to me. One of the nurses, Courtney, set up her laptop for me so I could watch the basketball.”
“The staff always made sure I was OK, urging me to get up and do my physio. They would constantly encourage me and talk about the plan to get me to the ward. They would keep telling me I was doing well, which meant a lot,” Mark explained.
“And the reassurance for my wife, Wendy – there were times she rung at three in the morning – and one nurse spoke to Wendy for about 40 minutes. There was no such thing as no time for you.”
Even though he was admitted during the height of the second wave of COVID-19 in Victoria and staff were required to wear full PPE, Mark was impressed with the excellent care he received, as well as impressed at his surroundings in our state of the art ICU.
“There were no gaps in care and no excuses from the staff – even though they were wearing gowns and masks – everything was delivered as promised,” he explained.
Mark expressed his sincere appreciation of the ICU team and was keen to return to Northern Hospital to personally thank each and every staff member who was involved in his care.
Narkitaa Van Ekeren, ICU Nurse Unit Manager, and her dedicated team welcomed Mark – who was fighting fit – and Wendy to the unit to say thank you.
“We were delighted to welcome Mark back to visit the ICU. It isn’t often we get to see the progress our patients make after transfer to the ward. Moments like this leave a lasting impression on many nurses, making us proud,” Narkitaa said.
“We have invited Mark and Wendy back to assist with the planning and development of the Intensive Care Long Stay Procedure, and we look forward to their input and ideas for our soon-to-be opened outdoor space,” Narkitaa added.
In an interesting twist of fate, Mark was recently also pleased to see one of the dedicated nurses who cared for him during his time in ICU at the gym they both go to.